Omicron is the newest virus to endanger indigenous communities, but it will not be the last, argues Dr. Shazia Tabassum Hakim, a professor of microbiology and biomedical sciences at Diné College.
By Shazia Tabassum Hakim

As of December 10, 2021, 17:05 GMT, a total of 5,307,847 people have died from the coronavirus COVID-19 outbreak; there are currently 269,112,118 confirmed cases in 222 countries and territories, according to the reference website Worldometer. Compounding the crisis is the new, potentially more transmissible variant of SARS-CoV-2-B.1.1.529, known as “Omicron,” which has been making headlines since November 26, 2021. Initially reported by South Africa, more than 1,500 cases have since been detected in more than 57 countries. Although South Africa was the first country to report this new variant, Dutch public-health officials stated that they detected Omicron in two COVID test samples taken in the Netherlands on November 19 and 23, suggesting that this variant was already circulating in Europe. Many countries have adopted travel bans to more than 14 countries, including but not limited to South Africa, Hong Kong, Botswana, Lesotho, Eswatini, Zimbabwe, Namibia, and France, along with many other travel-related restrictions on air travel and land border crossings.
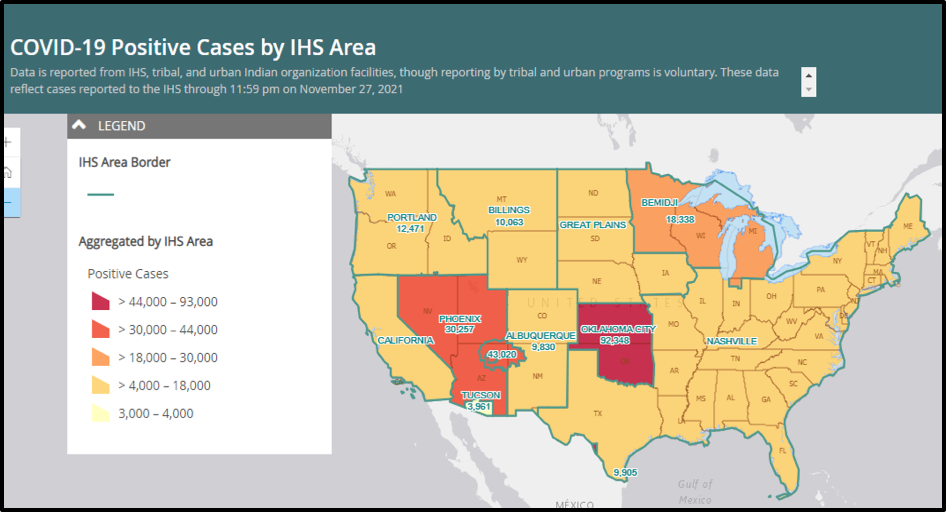
According to the CDC, the first U.S. case of the “Omicron variant” was identified on December 1. As of December 10, 43 confirmed cases have been reported across the country; 22 states have reported at least one case. The variant is not only infecting the vaccinated population, including those who had an additional or booster dose, but re-infecting those who have documented previous SARS-CoV-2 infections. Though the reported symptoms are comparatively mild, the long-term impact is not yet known, reinforcing the need for vigilance and planning within Native communities. If we look at the current number of cases reported by the Indian Health Services (IHS), it is very clear that the situation is not over. There is a continuous surge in new cases, especially within the Southwest and Midwest regions, which are home to the Navajo, Hopi, Yavapi, Tohono O’odham, Zuni, Pueblo, Pawnee, Concho, Chickasaw, Cherokee, Shawnee, Seminole, Kiowa, Choctaw and many other tribes. Thankfully, at present, we do not have any reported Omicron cases in indigenous communities, but how long will they be spared?
Omicron?
We have heard Alpha, Beta, Theta, Delta, Epsilon and now this Omicron variant. According to Merriam Webster, “Omicron” is the fifteenth letter of the Greek alphabet (om·i·cron | ˈä-mə-ˌkrän |ˈō-mə-ˌkrän | British ō-ˈmī-krän ) with the meaning small “O”. To name variants, the World Health Organization (WHO) uses Greek letters because they are easier to communicate than scientific designations like B.1.617.2. According to WHO, the thirteenth and fourteenth Greek letters (nu and xi) were skipped over because “nu” sounds like “new,” and “xi” is also a common surname. WHO’s best practices for naming new diseases, developed in conjunction with FAO (Food and Agricultural Organization of United Nations) and OIE (World Organization for Animal Health), suggest avoiding names that cause “offense to any cultural, social, national, regional, professional or ethnic groups.”
Phylogenetic and corresponding taxonomic characterization is central in microbial genomics. Evolutionary connection among clusters of organisms, particularly molecular phylogenetics uses sequence data to understand these connections for both organisms and the inheritable factors i.e. genes they retain. All variants and mutated organisms are given scientific names that signify their lineage, parentage, and the sequence of evolution. With reference to COVID-19, the “Technical Advisory Group on SARS-CoV-2 Virus Evolution (TAG-VE)” is an independent group of experts that periodically screens and evaluates the evolution of SARS-CoV-2 and assesses if specific genetic changes, mutations, and combinations of mutations might alter the behavior of the virus. The TAG-VE was convened on November 26, 2021 to evaluate the SARS-CoV-2 variant: B.1.1.529
Zhou et al reported in 2020 that SARS-CoV-2 is a member of Betacoronavirus of subgenus Sarbecovirus. This puts SARS-CoV-2 in the same genus as the Middle East respiratory syndrome coronavirus (MERS-CoV) and same subgenus as SARS-CoV (SARS Virus; 2003). By comparing the novel 2019 coronavirus to other human corona viruses (HCoV) and already recognized animal corona viruses, scientists gain insight into how the viruses pass on a disease to people, and understanding into potential regions for testing. There are multiple hypothesis scientists are working on to find the answers regarding the emergence of “Omicron,” including: the animal source, “Cryptic spread” in an unmonitored region, incubation in an immuno-compromised person, or possible intermixing with common cold virus genome. Low socio- economic conditions, multiple environmental factors and selective pressure should also not be excluded.
According to WHO, a SARS-CoV-2 VOI (variant of Interest) is a SARS-CoV-2 variant with genetic changes that are predicted or known to affect virus characteristics such as transmissibility, disease severity, and immune escape, diagnostic or therapeutic escape? Additionally, it has been identified as causing significant community transmission or multiple COVID-19 clusters in multiple countries with increasing relative prevalence alongside increasing number of cases over time, or other apparent epidemiological impacts to suggest an emerging risk to global public health.
A SARS-CoV-2 VOC (Variant of Concern) is a SARS-CoV-2 variant that meets the definition of a VOI and, through a comparative assessment, has been demonstrated to be associated with one or more changes of global public health significance, including: an increase in transmissibility or detrimental change in COVID-19 epidemiology, or an increase in virulence or change in clinical disease presentation, or a decrease in effectiveness of public health and social measures or available diagnostics, vaccines, and therapeutics.
This scientific background of “Omicron” helps us to understand that this is a continuous process; all living creatures, including microorganisms, have to adopt in order to survive. They are changing, mutating and adopting themselves according to their survival needs. We cannot stop them from adopting. What we can do is to prepare ourselves.
Important contributing risk factors behind the spread of infectious diseases among indigenous and underrepresented communities include low socio-economic conditions associated with poverty, limited economic development, limited healthcare infrastructure, and low literacy rates. Day-to-day household activities, as well as medical, agricultural or environmental practices, also contribute to the emergence of new pathogens and transmission from non-pathogenic populations; additionally, switching between various hosts cannot be neglected. Glasmeier (2006) has identified six major distressed regions of poverty within the United States: Appalachia, the Mississippi Delta, other areas of rural poverty especially in the American South, Native American tribal lands, the borderlands between the United States and Mexico, and highly segregated urban areas including mostly black metro areas adjacent to the Great Lakes and in the Northeast. These are the regions where we find the majority of positive cases.
We also understand that limited education directly correlates with poverty. Improving educational opportunities will directly impact the socioeconomic conditions of our indigenous communities. It logically follows that we need to develop our educational institutions so they can meet the needs of our students in a changing world. We must think about how we are able to use our traditional Ecological Knowledge (TEK), along with the latest available technologies, to make the world better for our future generations. We must equip our youth with scientific knowledge and advanced technologies (STEM) wrapped in traditional knowledge (TEK). In 1968 Diné College opened its doors as the “first tribally controlled post-secondary institution,” marking a new era of self-determination for Native American students. This historic event led to the 1971 “Navajo Community College Act” and, in 1978, the “Tribally Controlled Community College Assistance Act,” paving the way for new tribal colleges. Since then, Tribal Colleges and Universities (TCUs) have grown to include 40 institutions spread across 16 states, serving over 40,000 students – approximately 80% of whom are American Indian or Alaska Native.
Besides conferring certificate, associate or baccalaureate degree seeking programs, these institutions are offering programs such as traditional skills, language and reading instruction, computer literacy courses, health and wellness classes, and leadership development and entrepreneurship courses, just to name a few. The COVID-19 pandemic simply heightened the need for development of more healthcare related programs, all of which contribute to tribal sovereignty. Participation in these programs is growing day by day. For example, two programs at tribal colleges and universities (TCUs) in North Dakota and Montana received $1.125 million grant through American Indian College Fund to help Native American student success in careers in healthcare and education. As compared to the colleges’ early years, a number of tribal colleges have facilities to offer two-year or four-year degree programs, six colleges are offering master’s level programs, while one is working to finalize its doctoral program. Funding coming through USDA/NIFA/ TCRGP, NSF-TCUP, NSF- TEA Center, NSF-SGR, NIH and other programs that is directly impacting the quantity and quality of tribal colleges and universities, while, focusing more on STEM and healthcare related programs to prepare future native scientists, healthcare professionals and leaders.
The winter season is already here; influenza and multiple variants of SARS-COV-2 are around, along with many other coronaviruses that infect mildly. They are adapting, they are changing, but so are we–by learning, from every new germ, every new variant, how to defeat them through science and education–through our traditional knowledge, competence, wisdom, and resilience. Similar to the flu virus, these SARS-CoV-2 variants will continue coming. This will not be the last germ for indigenous communities to deal with. What is needed is a stronger vigilance system and greater preventive measures, including a need to prepare the locally trained indigenous workforce. The people should continue using all recommended standard precautionary measures and practicing the traditional wisdom that they gain from their elders to tackle what we have to unfold next.
References:
- https://www.worldometers.info/coronavirus/coronavirus-death-toll/
- “Omicron.” Merriam-Webster.com Dictionary, Merriam-Webster, https://www.merriam-webster.com/dictionary/omicron. Accessed 1 Dec. 2021.
- Zhou, P. etal. 2020. Discovery of a novel coronavirus associated with the recent pneumonia outbreak in humans and its potential bat origin. BioRxiv http://dx.doi.org/10(2020.01):22-914952
- » http://dx.doi.org/10(2020.01):22-914952
- Ziemert, Nadine, and Paul R Jensen. “Phylogenetic approaches to natural product structure prediction.” Methods in enzymology vol. 517 (2012): 161-82. doi:10.1016/B978-0-12-404634-4.00008-5.
- McNulty, K. P. (2016) Hominin Taxonomy and Phylogeny: What’s In A Name? Nature Education Knowledge 7(1):2
- https://www.who.int/news/item/26-11-2021-classification-of-omicron-(b.1.1.529)-sars-cov-2-variant-of-concern.
- https://www.who.int/news/item/26-11-2021-classification-of-omicron-(b.1.1.529)-sars-cov-2-variant-of-concern.
- https://www.who.int/news/item/26-11-2021-classification-of-omicron-(b.1.1.529)-sars-cov-2-variant-of-concern.
- https://www.cdc.gov/media/releases/2021/s1201-omicron-variant.html.
- https://nymag.com/intelligencer/article/what-we-know-about-the-omicron-b11529-covid-variant.html
- Glasmeier AK. 2006. An Atlas of Poverty in America: One Nation, Pulling Apart, 1960–2003. Distressed Regions Section. New York and London: Routledge Taylor & Francis Group. 51–80.
- https://www.cdc.gov/mmwr/volumes/70/wr/mm7050e1.htm?s_cid=mm7050e1_w
Story published December 14, 2021
• • •
Enjoyed this story? Enter your email to receive notifications.
